Health
Breast & Cervical Cancer
Rental Housing
Violent Crime
Self-Sufficiency
Basic Needs
Physical Activity
Nutrition
Minorities
Mental Health
Childhood Immunizations
Heart Disease
Health Care Coverage
Feeling Well
Traffic Crashes
Communicable Diseases
|
Why This Measure?
American women have a one-in-eight risk of developing breast
cancer over an average lifetime. Our lead indicator focuses on mammography because it has
been shown to reduce deaths by 26% for women aged 50 and over (althouth it does not appear
to reduce breast cancer mortality for premenopausal women) (Personal Health: A
Multicultural Approach, 1995). Small tumors are easier to detect by x-ray against the
higher content of fatty breast tissue typical of older women, as opposed to dense, fibrous
breasts. With early detection, treatment can be more successful. The indicator is also a
good gauge of the overall effectiveness of the health care delivery system.
Lead Indicator:
Selected Montana Women Getting Breast Exam and Mammograms
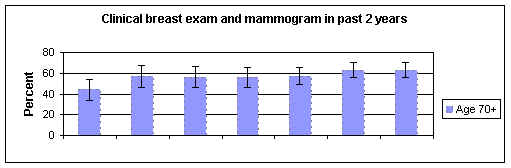
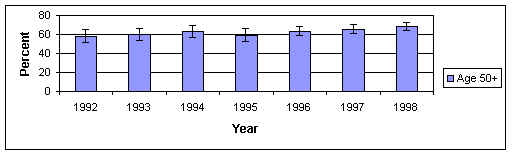
Source Montana BRFSS 1998
Missoula County Population Estimates (July 1998) By
Age and Gender (useful in translating percentages and rates into actual numbers in certain
age categories, or vice versa) Missoula County Population
Trend Suspect Better Data Rating Available Reliable
Relevant
How are we doing?
In terms of mammograms, we appear to be doing well. We have
surpassed the Healthy People 2000 goal of 60%. But that still leaves nearly three in 10
women over 50 whom we still need to reach. Current mammogram guidelines
recommend that women over 20 do self-exams every month, receive clinical breast exams
between 20-40 every three years, receive an initial mammogram at 35, and annual mammograms
beginning at 40. 23% of breast cancer occurs in women under age 50. Mammograms miss
about 15% of breast cancers. (Dr. Judy Schmidt) Of Missoula women over 50, 58% got a
mammogram within the past year during1996.
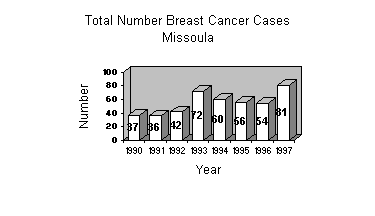
Source: Montana Central Tumor Registry,
MDPHHS, Vital Statistics
Breast
Self-Exams
Nine out of 10 women discover tumors through regular breast
self-exam, and 80% of those tumors are benign (The Impact of Cancer on Montana, Part 1:
Cancer Fact Book, 1995). However, tumors detected in this manner are usually larger and in
a later stage of growth.
Why
Don’t Some Missoula Women Get Mammograms?
In six Missoula focus groups, reasons for not getting mammograms
included:
- Lack of financial resources.
- Disbelief of media messages.
- Preference for female health care providers.
- Great fear of cancer.
- Strong influence of female peers and family.
- "Fear factors," embarrassment, pain, and discomfort.
(Six Focus Groups, PHC, 1995)
Risk Factors for
Breast Cancer
Over 80% of women having breast cancer have NO identified
risk factors. The primary risk factors are being a woman and getting older. Over 75% of
breast cancer cases are in women over 50, and the risk increases with age. All women are
at risk and need to have yearly mammograms, clinical breast exams, and do monthly breast
self-exams. Over 95% of women diagnosed with breast or cervical cancer survive when it is
found early. It is not a death sentence - early detection is very important to finding
these cancers when they can be easily and successfully treated. (Karen Cater, DPHHS)
Risk factors associated with family history account for about 5%
of breast cancer cases. (Dr. Judy Schmidt) Other factors correlated with some
increased risk include early menarche, late menopause, never bearing children or late age
at first birth (Cancer Facts and Figures, American Cancer Society, 1995). The levels and
types of fat common in the American diet, moderate alcohol consumption, and obesity have
also been associated with higher breast cancer rates, as well as lack of exercise (4 hours
per week are necessary) (The Impact of Cancer on Montana, Part I: Cancer Fact Book, 1995).
Additionally, women with lower incomes (less than $20,000 annual household income) are
less likely to have had a breast physical exam than women with higher incomes (MT BRFSS,
1996).
Resources for Missoula
Women
The Montana
Breast and Cervical Health Program has produced a brochure called
"side-by-side" that summarizes services of the MBCHP, the American Cancer
Society, and the Montana Komen Race for the Cure, as well as more websites.
The Montana Breast and Cervical Health Program has an
administrative site in Missoula offering yearly mammograms, clinical breast exams,
education, and regular Pap tests to uninsured or underinsured women ages 50 through 64.
Income to qualify is up to and including 200% of poverty (a woman in a one person
household can earn up to $7.92 per hour in a full-time job andqualify). The Missoula site
serves Missoula, Sanders, and Ravalli counties. Enrollment of providers is currently being
done, so there should be providers available in each county to serve qualified women.
Daphne Evans is the coordinator in the Missoula area, located at Partnership Health
Center.
|